
Before Ayla was born, she had already made history.
Diagnosed prenatally with a rare genetic disorder called Pompe disease, Ayla received a world-first in-utero treatment at The Ottawa Hospital last year. The often-fatal disease had already taken the lives of two of her siblings in early childhood.
Today, Ayla is healthy and happy. In June, she celebrated her first birthday. “We had all of our family over,” says Ayla’s mother, Sobia Qureshi. “It was a big deal for everyone because the loss of our two older children was felt by them all. But to see Ayla developing like this, it’s sometimes hard to remember that she has Pompe.”
What is Pompe disease?
Pompe disease is an inherited genetic disorder that weakens muscles throughout the body, especially in the heart and skeleton. People with Pompe disease lack an enzyme called acid alfa-glucosidase, which breaks down the complex sugar glycogen so it can be used for energy. When too much glycogen builds up in the muscle cells, the cells become damaged and the muscles lose their function. The disease is rare, occurring in about 1 in 40,000 births.
Without treatment, affected children usually die in the first year of life. Children born with this disease require life-long enzyme replacement therapy, but many signs of the disease can already be present at birth.
New treatment offers new hope
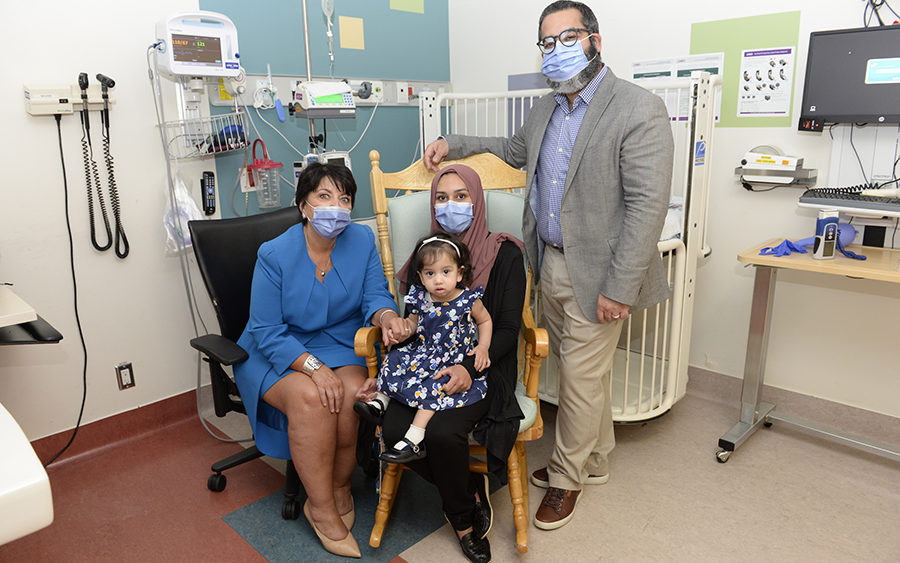
Shortly after receiving the diagnosis that her unborn baby was affected with Pompe disease, Sobia asked her family doctor to refer her to Dr. Karen Fung-Kee-Fung, Maternal Fetal Medicine Specialist at The Ottawa Hospital.
“I had seen her once in the past, and I really liked her,” says Sobia. “And I’m really glad I was referred to her.”
In another fortunate turn of events, a promising new clinical trial had just been approved at UC San Francisco.
Instead of starting Ayla’s treatment after she was born, the idea behind the trial was to first treat her in utero. This early intervention would hopefully limit the damage caused by the disease and prevent the vulnerable newborn from developing potentially serious immune reactions to the medication.
Dr. Fung-Kee-Fung collaborated with Dr. Pranesh Chakraborty, a metabolic disease specialist at CHEO who has provided pediatric care to the family for years. The two physicians quickly got Sobia approved for the trial.
World-first care close to home
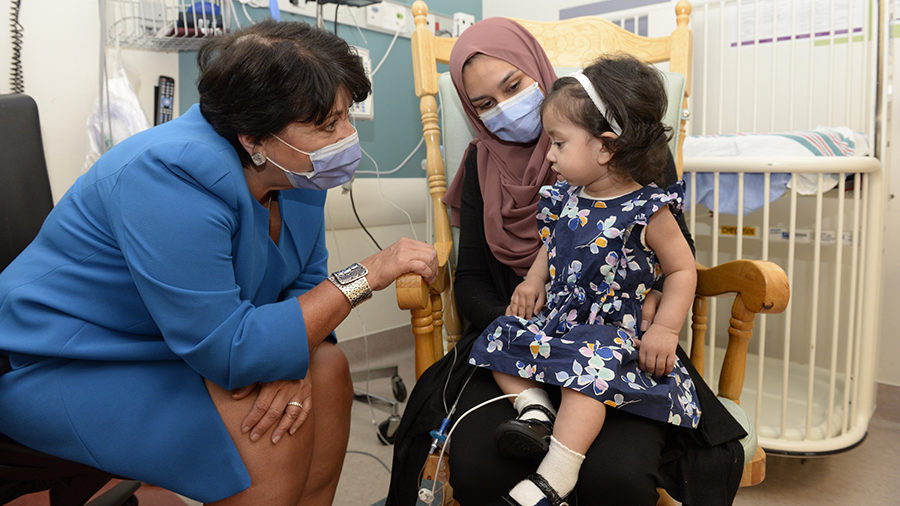
The plan originally called for Sobia to travel to California for six sessions of prenatal enzyme replacement therapy, one every two weeks. But COVID-19 restrictions, coupled with caring for her two children, made travel impractical.
“It became apparent that we had to think of a plan B—and that was to offer the treatment here,” says Dr. Fung-Kee-Fung.
After consulting with the clinical trial team at UC San Francisco and Pompe disease experts at Duke University, Dr. Fung-Kee-Fung and the Maternal Fetal Medicine team got the green light to perform the treatment at The Ottawa Hospital.
Dr. Fung-Kee-Fung administered the six therapy sessions with Dr. Felipe Moretti, head of the hospital’s Maternal Fetal Medicine Division. Although this treatment is new, the procedure for delivering the enzyme is the same used for other in-utero therapies, which Dr. Fung-Kee-Fung has performed at The Ottawa Hospital for more than 30 years.
“We were privileged to be part of this unique collaboration,” says Dr. Fung-Kee-Fung. “UC San Francisco and Duke University provided the novel science behind this approach to therapy. And in Ottawa, we had the experience and the team to take advantage of this opportunity and provide Ayla with this life-saving treatment locally.”
Not only did Dr. Fung-Kee-Fung administer Ayla’s treatment, but she also delivered her, much to Sobia’s joy. “I was hoping that she would deliver the baby, and she did!” says Sobia. “I wouldn’t have had it any other way.”
At 17 months old, Ayla is thriving

Today, Ayla is receiving standard postnatal therapy at CHEO from Dr. Chakraborty. Her heart and body are growing and working normally. Just before her first birthday, she started walking—and her parents are having a hard time keeping up with the active toddler.
“The new thing she’s learned is climbing onto our sofas,” Sobia says with a laugh. “I don’t think I’ve had to watch any of my kids as much as we have to watch Ayla.”
Although Ayla’s future is uncertain, the treatment has given her family hope. “We don’t know what things are going to look like in the next five, 10, 20 years,” says Sobia. “I hope this trend continues and she does amazing.”
For many more families, a brighter future could be on the horizon

“This treatment offers hope to so many other families who have been impacted by this disease,” says Dr. Fung-Kee-Fung. “But there are many people just like Sobia who won’t be able to travel to the U.S. to receive this treatment.”
That’s why the clinical and research teams at the Ottawa Hospital Research Institute and the CHEO Research Institute have collaborated and submitted a grant proposal to the Canadian Institutes of Health Research to make The Ottawa Hospital a trial site for this groundbreaking treatment.
The future could also see other genetic disorders treated the same way.
“This is the tip of the iceberg,” she says. “If we are able to successfully administer an enzyme to our fetal patients for this disease, there are other families out there affected by similar genetic diseases who will most likely be able to benefit from a treatment such as this.”

Support patient care and research at
The Ottawa Hospital
You might also like…
Construction underway on long-term care home at Riverside Campus
Caring for our seniors takes a village. The Ottawa Hospital and Schlegel Villages have partnered for The Village of Riverbank Terrace, a 256-bed long-term care home at our Riverside Campus. Find out how this new home will help fulfill the needs of Ottawa’s growing community of seniors.
Dr. Kathleen Gartke appointed to the Order of Ontario
The Ottawa Hospital is proud to share that Dr. Kathleen Gartke has recently been appointed to the Order of Ontario, the province’s highest honour. A pioneering orthopedic surgeon, Dr. Gartke has been recognized for advancing patient care and women’s leadership in medicine.
Reimagining hospital food: How The Ottawa Hospital is transforming the patient mealtime experience
In 2024, we launched the trial phase of our Patient Food Transformation Project. The goal was to see if it is possible to improve the overall nutrition and quality of food we serve to our patients, while increasing bedside hospitality, enhancing the overall sustainability of our food services, and not increasing operational costs. Our trial wrapped in 2025 with very promising results.
How we’re helping over 1,400 paramedics enhance patient care and safety
The Regional Paramedic Program for Eastern Ontario (RPPEO) is on a mission to enhance what happens after you dial 911. Here are three new ways this team is helping paramedics deliver better, safer care to their patients.
New program fills gap in care for teens and young adults with cancer
For young people, a cancer diagnosis can disrupt their education, careers, relationships and family-building goals. Our Adolescent and Young Adult (AYA) Cancer Program supports AYAs on their cancer journey, complementing the care provided by their care team.
Less time charting means more time with patients: How The Ottawa Hospital is using AI to support patient care
“I’m seeing and treating more patients.” Find out how DAX Copilot, a powerful AI assistant, is helping our physicians cut down on paperwork, improve their own well-being and spend more time with patients.


 To reset, hold the Ctrl key, then press 0.
To reset, hold the Ctrl key, then press 0.





