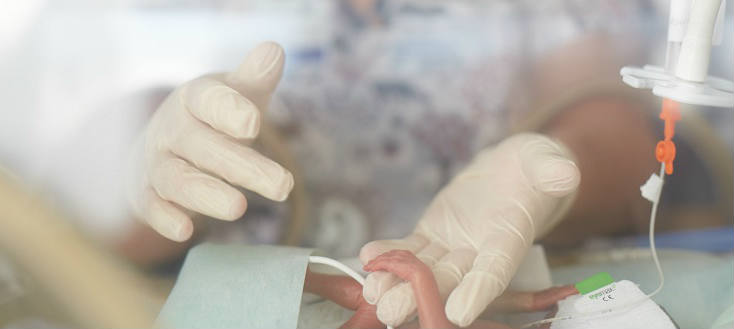
Baby Abigail was born at 22 weeks’ gestation, weighing barely over a pound.
In the isolette, a tiny, week-old baby lifts her index finger-sized arm. Baby Abigail weighs 498 grams – barely over a pound. She was born four months early, at 22 weeks, 6 days’ gestation.
Extremely premature babies like Abigail are at high risk of dying, regardless of medical intervention, and of having neurodevelopmental and other physical disabilities. A few years ago, those born at 22 weeks generally received palliative care, and passed away naturally after birth. However, the hospital has a new approach based on research and discussion with parents.
Abigail’s mother, Dena Larabie, was informed of the risks and potential developmental issues that extreme preemies face.
“I was told that, being born at 22 weeks, her rate of survival is low but possible,” said Larabie. She was part of a shared decision-making process, new to The Ottawa Hospital. As a result, she chose to have Abigail receive intensive care, with hope that she would survive.
When neonatologist Dr. Gregory Moore returned after working for a year at a hospital in Melbourne, Australia, he noted that extreme preemies in Australia were reported to have better survival and lower neurodevelopmental disability rates than those quoted by neonatologists at The Ottawa Hospital. He wondered why, considering the similar level of care in Melbourne. He noted that the neurodevelopmental disability rates used here were based on one study from Britain. Dr. Moore felt this wasn’t enough information.

Dr. Gregory Moore, a neonatologist at The Ottawa Hospital and CHEO, and an Assistant Professor at the University of Ottawa, examined a baby born at 22 weeks’ gestation. “The NICU team at The Ottawa Hospital may attempt intensive care for some infants born as early as 22 weeks if the parents strongly believe that it’s in their infant’s best interests,” he said. “We also very much support parents who choose palliative care.”
“Along with some colleagues, I put together a systematic review of published literature that followed babies born between 22 and 25 weeks who were alive at school age, and examined certain neurodevelopmental disabilities,” said Dr. Moore. “The studies looked at the children’s cognitive abilities, their IQ test scores; how they think, talk and communicate; their motor skills, such as how well they walk; and their likelihood of blindness and deafness.”
His research showed these extreme preemies ended up doing better than what was noted in the British study. Other research showed that other factors affect how well a baby does, such as greater birth weight and mothers who received antenatal steroids.
“It made us realize that some babies born at 22 or 23 weeks could do better than some babies born at 24 or 25 weeks, depending on the various factors,” said Dr. Moore.
He led a 16-person interdisciplinary working group of neonatologists, nurses, an ethicist, social worker, and parents, to create a shared decision-making guideline and a tool. These help parents make informed decisions about whether they want their extremely premature baby to receive intensive care or palliative care. The shared decision-making approach ensures that the family’s life experience, culture, religion, and values play major roles. The medical team explains the statistics and prognosis regarding survival and neurodevelopmental disabilities to the family. This gives them an idea of what they could face if their child survives and has disabilities. The goal is to give parents truthful and accurate information, so that they are fully informed before making a decision.

NICU Clinical Manager Janet Brintnell discussed care of a baby born at 22 weeks’ gestation with Registered Nurse Joanne Major.
Not long after the team implemented the shared decision-making process, a baby was born at 22 weeks’ gestation, and the parents asked the NICU team to try intensive care to help their baby.
“We didn’t really know how to care for this baby, as we’d never cared for one this premature,” said Janet Brintnell, Corporate Clinical Manager for the Neonatal Intensive Care Unit and the Special Care Nursery. “These extreme preemies are at risk for so much. Their skin is so fragile. Even our sheets are too rough for their skin. We didn’t know the extent of the care needs these tiny babies had.”
Sadly, the baby lived only a short time, but the family was thankful that the NICU team had made such efforts, and was grateful to have been a part of their child’s brief life.
“We identified a whole bunch of issues and that made us work really hard to ensure the best possible conditions for these babies,” said neonatologist Dr. Brigitte Lemyre. “Before these guidelines, we had no survivors under 23 weeks because we almost never attempted resuscitation. Now, if some parents wish, after hearing all the information, we do attempt resuscitation and intensive care.”

“Since the guideline, we have had two babies survive at 22 weeks’ gestation, which was previously unheard of here in Ottawa,” said neonatologist Dr. Brigitte Lemyre. “They are both home and doing well, though it is too early to determine their neurodevelopmental outcome. One is 18 months. The other is 11 months.”
“Since the guideline, we have had two babies survive at 22 weeks’ gestation, which was previously unheard of here in Ottawa,” said neonatologist Dr. Brigitte Lemyre. “They are both home and doing well, though it is too early to determine their neurodevelopmental outcome. One is 18 months. The other is 11 months.”
Brintnell said that what they learned has helped them develop better treatment plans, which resulted in them seeing an improvement in the 25- to 26-week-old preemies. Improving the care for the smallest has improved the care for the bigger babies.
“In the end, we’ve changed from some black-and-white decisions based on gestational age to a prognosis-based approach,” said Dr. Moore. “Families are prepared and that’s the purpose of shared decision-making.” He has spoken about these practices at conferences. Other hospitals are now looking to The Ottawa Hospital for guidance in treating babies less than 25 weeks.
Though her chance of survival is uncertain, if all goes well, baby Abigail will be in the NICU until her due date in March 2018, then go home to her family.
The Ottawa Hospital is raising funds to renovate its NICU, which is critical for babies like Abigail to receive the most up-to-date treatments to give them the best chance at surviving, thriving and growing up.

Support patient care and research at
The Ottawa Hospital
You might also like…
Living with chronic pain? This online tool offers help — and hope
The Power Over Pain Portal is a free virtual resource hub designed to help empower youth and adults living with chronic pain through education and peer support.
From survivor to supporter: Peer volunteers bring hope to patients recovering from stroke
Drawing on their own lived experiences as stroke survivors or caregivers, volunteers with March of Dimes Canada’s After Stroke Hospital Peer Connections program offer emotional support to those just beginning their recovery journey. Discover the difference they’re making and learn about how you can request support for a loved one — or become a beacon of hope yourself.
Sign language interpretation services at The Ottawa Hospital: 5 FAQs
Do you require a sign language interpreter when you come to The Ottawa Hospital? For patients who are Deaf or hard of hearing, we provide both American Sign Language (ASL) and Langue des Signes Québécoise (LSQ) interpretation services at no cost. Before your next appointment with us, find out everything you need to know.
Caring for your newborn and yourself: A post-birth guide for parents
Have you just given birth? Are you expecting soon? In this series of videos, Registered Nurse Samantha Adams shares essential advice for those early days at home.
Baby on board: Nurses jump into action to help deliver baby during flight
When a woman went into labour in the middle of a seven-hour flight, Eunice and Lindsey immediately volunteered their services. The two neonatal intensive care nurses had to rely on their experience — and a little improvisation — to help deliver and resuscitate a baby girl.
Watch: NICU babies and staff receive special Challenge Coins from Ottawa Fire Services
This may be the feel-good video of the year! After helping carry our tiniest patients out of harm’s way on October 27, firefighters return to the General Campus NICU to present staff, families and babies with a special gift.


 To reset, hold the Ctrl key, then press 0.
To reset, hold the Ctrl key, then press 0.





